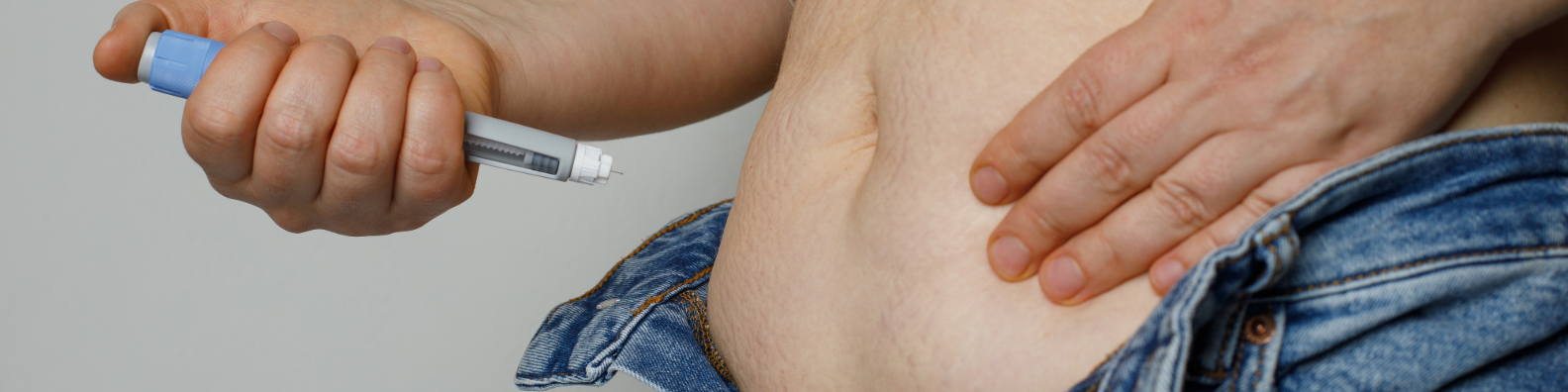
Americans are increasingly desperate to lose weight as our national obesity rate increases. The current mania for injectable weight loss drugs like Ozempic reflects this desperation. However, is there something lurking behind the headlines?
What is Ozempic?
Ozempic (i.e., semaglutide) is a member of a class of drugs known as incretin mimetics. Incretin mimetics enhance insulin release from the pancreas. Such drugs were initially developed to help treat type 2 diabetes by increasing their insulin levels to help drive more blood glucose into muscle cells, thus lowering HbA1c levels.
Ozempic is an incretin mimetic. It was developed to activate the hormone receptor activated by the natural hormone known as Glucagon-like protein 1 or GLP-1 (1). It was found in clinical trials that the higher the dose of Ozempic, the greater the weight loss. Consequently, the same drug (semaglutide) was rebranded as a weight-loss drug (i.e., Wegovy) but now with a higher dose than Ozempic for treating diabetes. The FDA recently approved Wegovy for weight loss.

Differences between weight loss and fat loss
FDA approval for any weight loss drug is only based on weight loss, not fat loss. The initial data using higher doses of semaglutide (the generic name of the compound used in both Ozempic and Wegovy) shows that about 40 percent of weight loss in non-diabetic overweight individuals was from loss of muscle mass (2). Furthermore, once the injections were stopped, there was a rapid regain in weight (3).
How do Ozempic and Wegovy work?
Incretin mimetics increase insulin levels at a lower dosage, which usually increases hunger. Yet, Ozempic and Wegovy decrease appetite. This seemingly paradoxical result comes as the higher doses of these drugs activate GLP-1 receptors in the brain’s hypothalamus. It should be noted that GLP-1 is stimulated by adequate dietary protein in a meal.
In addition, these higher drug doses also slow down gastric emptying. This effect is known as gastroparesis, which usually occurs when the vagus nerve that connects the gut to the brain is damaged or stops working.
Ingested food usually exits the stomach within 30 minutes to two hours after eating. The time that food sits in the stomach can be significantly extended if you develop gastroparesis. Therefore, one of the common side effects of these drugs is the development of nausea if you try to increase food intake. Furthermore, these drugs also slow down the peristaltic action of the intestine (4), so it becomes painful to consume more food unless the small intestine is finally cleared from the previous meal, which usually takes about five hours under normal conditions. This residence time for food in the gut becomes longer in the presence of these drugs because they slow down the normal peristaltic action that moves food through the gut. The combination of all these effects is why these drugs restrict calorie intake.
This concept is essential as calorie restriction activates AMPK (the master regulator of your metabolism) that causes fat loss, not the injected drugs. The AMPK activation that generates the actual fat loss is simply a side benefit of high-dose Ozempic or Wegovy used to decrease appetite.
The bottom line, once you stop injecting these drugs, weight regain immediately begins to reoccur. However, the regain of weight will likely be due primarily to new fat accumulation since it takes time to rebuild muscle, which requires adequate protein and exercise. Thus, you are potentially worst off once you stop taking these drugs because the increased body fat accumulation will likely increase insulin resistance. This increases your future health risk since insulin resistance drives many chronic diseases such as type 2 diabetes, heart disease, and Alzheimer’s.
A growing hormonal arms race
Ozempic and Wegovy are wildly successful drugs. However, these drugs only affect the GLP-1 receptor in the hypothalamus. What if you could make a drug that interacts with more hormone receptors to reduce hunger? Mounjaro (i.e., tirzepatide), made by Eli Lilly, is just such a drug as it affects the receptors for two hormones in the brain: GLP-1 and GIP (Gastric Inhibitory Protein). Like GLP-1, GIP is also released by dietary protein. As you might expect, Mounjaro generates more significant weight loss than either Ozempic or Wegovy (5). The reason is that GIP is more effective than GLP-1 in slowing down gastric emptying, thus making it difficult to consume food without creating nausea.
If affecting two hormones is better than one, what about affecting three hormones involved in satiety? The newest Eli Lilly weight loss drug (i.e., retatrutide) does that (6). It affects three satiety hormones: GLP-1, GIP, and glucagon. Remember that incretins were initially developed to stimulate the release of insulin in type 2 diabetics to increase blood insulin levels to reduce blood sugar levels. However, increasing blood insulin in non-diabetics will cause increased fat accumulation, slowing down fat loss. The solution is to stimulate glucagon release from the pancreas, which will lower insulin levels. Not surprisingly, you get even more significant weight loss with these multi-hormone receptor agonists but with potentially more side effects (7). Not surprisingly, glucagon release from the pancreas is also stimulated by dietary protein.
Alternatives to Ozempic and other hormone receptor agonist drugs
These weight loss drugs must be used for a lifetime to keep the lost weight from returning. Great news for the drug companies, but not so good for the patient. So, is there an alternative?
First, remember that dietary protein is the natural stimulus for releasing each of these hormones that suppress appetite. Second, to achieve fat loss, you must reduce insulin resistance, and the underlying cause of insulin resistance is dietary inhibition of AMPK (9). So, could a dietary system that provides adequate dietary protein and increases AMPK activity provide a pathway for fat loss without loss of muscle mass?
Such a dietary system exists and has been shown to do exactly that. That dietary system is the Zone diet. The foundation for the Zone diet was first described in my book, The Zone, published in 1995 (10). The basic patent for using the Zone diet to reduce insulin resistance was applied in 1992 and issued in 2000 (11).
Since that time, I have continued to add several dietary enhancements to the basic concept to make the Zone diet an appropriate alternative to Ozempic, Wegovy, Mounjaro, and other potential hormonal-based drugs not only for weight loss but also as a treatment for diseases that are strongly associated with insulin resistance such as type 2 diabetes and heart disease.
How does the Zone diet work to increase GLP-1 release?
GLP-1 activates the POMC neurons in the hypothalamus to reduce satiety. But first, GLP-1 must be released in the gut in response to dietary protein, specifically by the L-cells located in the highest abundance in the distant part of the small intestine known as the ileum. The released GLP-1 then travels to the hypothalamus to interact with the POMC neurons to signal satiety. This short-term effect must be repeated at every meal if one wants continued satiety. Of course, that same dietary protein at a meal that stimulates GLP-1 release also causes the release of both GIP and glucagon.
Another benefit of consuming enough dietary protein at a meal is that it stimulates another satiety hormone released from the gut known as PYY (12). PYY also inhibits hunger. Thus, adequate dietary protein intake at a meal can stimulate four appetite-suppressing hormones compared to only one hormone stimulated by Ozempic or Wegovy.
Why not consume more protein at a meal for even greater satiety? There are two reasons. The first reason is that higher protein levels stimulate insulin release from the pancreas. Excess insulin secretion causes inhibition of AMPK activity which slows down fat loss (13). The second reason is that excess protein overstimulates the gene transcription factor mTOR, inhibiting AMPK activity (14). Any reduction of AMPK activity slows down the burning of stored body fat.
The ideal amount of protein you need at a meal to induce GLP-1 release without overstimulating mTOR is about 30 grams per meal. So, with the correct amount of protein at a meal, you can naturally generate four hormones germane to enhancing satiety activation.
However, you must balance that appropriate amount of protein with the correct amount of low-glycemic carbohydrates to maintain stable blood sugar levels. If the 30 grams of protein at a meal is balanced with carbohydrates rich in fermentable fiber, this allows the production of short-chain fatty acids (SCFA ) by gut microbes that further enhance GLP-1 release from the gut (15). The best carbs are low glycemic carbohydrates, primarily non-starchy vegetables, just like your grandmother told you to eat.
Thus, for every 30 grams of protein at a meal, you will need about 40 grams of fiber-rich carbohydrates to generate the maximum satiety effect. This is the foundation of the Zone diet’s patented ability to reduce insulin resistance, which is the key to losing excess body fat.
Another reason you also need a balanced protein-to-carb ratio at each meal is to maintain the dynamic balance of mTOR to AMPK to prevent loss of muscle mass. This because mTOR is critical to promoting the maintenance of muscle mass. Losing weight is counter-productive if much of that weight loss is muscle loss.
Bottom line: You need to stimulate GLP-1, GIP, glucagon, and PYY with adequate protein to stop hunger, restrict calories to activate AMPK to burn excess stored body fat, and yet generate enough mTOR activity to maintain muscle mass during your weight loss. It seems like Mission Impossible, but by following the Zone diet, it is possible to achieve this on a lifetime basis.
Thus, using the Zone diet as a lifetime dietary method to lose excess body fat and maintain (if not gain) muscle mass seems like a pretty good deal as opposed to injecting Ozempic and Wegovy, especially knowing that you will regain the lost weight once you stop the weekly injections.
Does the Zone reduce insulin resistance and increase fat loss while building muscle mass?
The Zone diet sounds great in theory, but does it work in humans? The answer is yes. The first demonstration of the Zone diet’s ability to increase glucagon and reduce appetite simultaneously was shown in 1999 at Harvard Medical School (16). This study showed that consuming two consecutive Zone meals based resulted up to a 46 percent reduction in calorie intake the next five hours after the second meal compared to using isocaloric meals with a different protein-to-carbohydrate ratio.
Another study published in 2010 in the New England Journal of Medicine demonstrated that after losing weight on an ultra-low 800-calorie-per-day diet for several weeks, only those subjects who followed a calorie-restricted diet (1700 calories per day) with a composition very similar to the Zone diet were able to maintain their lost weight for the next 26 weeks. Participants who followed diets with similar reduced calorie intake but with different macronutrient compositions regained much of their initially lost weight in the same 26-week period (17).
These early results were again confirmed in 2017, which was demonstrated under conditions of equal calorie restriction. One group used a more advanced form of food technology to enhance the release of GLP-1 from the ileum (18). This resulted in a 140 percent greater reduction in insulin resistance, more significant fat loss, and greater gain in muscle mass gain compared to the control group, who lost muscle mass and less body fat although consuming the same number of daily calories (18).
Further confirmation has come from two recent clinical studies. One study published in 2021 was a cross-over study that demonstrated that individuals who followed the dietary guidelines of the Zone diet had a more significant reduction in their levels of insulin resistance (the underlying cause of obesity) compared to those following a Mediterranean diet (19). Another study published in 2022 demonstrated that after losing weight on an ultra-low-calorie (800 calories per day) diet for eight weeks, the subjects switched to various calorie-restricted diets (about 1700 calories per day) with different protein-to-glycemic load ratios. Those subjects that mostly followed the macronutrient composition recommended by the Zone diet guidelines had the greatest reduction in insulin resistance (20).
What can be done to increase fat loss faster?
The answer is Metabolic Engineering®. Metabolic Engineering® is a more sophisticated approach to long-term metabolic control to lose excess body fat and reduce insulin resistance. Metabolic Engineering™ starts with the calorie-restricted Zone diet containing approximately 30 grams of protein per meal balanced by adequate levels of low-glycemic load carbohydrates and a dash of fat. You can achieve further reductions of insulin resistance via the activation of AMPK by supplementation with high-dose omega-3 fatty acids and polyphenols. Most individuals are deficient in these two nutrients. For example, a recent study published in 2023 demonstrated that 4.6 grams of EPA and DHA daily dramatically lowered insulin resistance in obese women within 30 days (21). Other studies have shown that consuming concentrated maqui berry extracts (rich in a subclass of polyphenol known as delphinidins) reduces HbA1c and oxidative stress (22,23). The reduction of these blood markers are an indication of increased AMPK activity.
While the Zone diet is a direct activator of AMPK, adequate intakes of omega-3 fatty acids and delphinidins are indirect activators of AMPK (24), thus amplifying the general benefits of long-term calorie restriction with the correct protein-to-carbohydrate balance.
Summary
Metabolic Engineering® represents an integrated systems biology approach to activate AMPK yet maintaining an appropriate mTOR/AMPK balance to generate a balance of burning stored body fat for energy while maintaining, if not, increase increasing, muscle mass without hunger or fatigue.
High-dose injectable hormone agonists like Ozempic and Wegovy represent a relatively crude approach to reducing hunger with numerous potential side effects. On the other hand, Metabolic Engineering® offers a more sophisticated approach to sustainable fat loss with no side effects. Although Metabolic Engineering® may require a little more discipline than a weekly injection of a weight loss drug, the long-term health benefits are dramatically better.
References
- Wilding JPH et al. Once weekly semaglutide in adults with overweight or obesity. Wilding JPH et al. N Engl J Med 384:989-1002 (2021) doi: 10.1056/NEJMoa2032183
3. Wilding JPH et al. Weight regain and cardiometabolic effects after withdrawal of semaglutide: The STEP 1 trial extension. Diabetes Obesity and Metabolism 24: 1553-1564 (2022) doi: 10.1111/dom.14725. - Nakatani Y et al.Effect of GLP-1 receptor agonist on gastrointestinal tract motility and residue rates as evaluated by capsule endoscopy. Diabetes Metab 43:430-437 (2017). doi: 10.1016/j.diabet.2017.05.009.
- Nauck MA and D’Alessio DA.Tirzepatide, a dual GIP/GLP-1 receptor co-agonist for the treatment of type 2 diabetes with unmatched effectiveness regarding glycaemic control and body weight reduction. Cardiovasc Diabetol 21:169 (2022). doi: 10.1186/s12933-022-01604-7.
- Coskun T et al.LY3437943, a novel triple glucagon, GIP, and GLP-1 receptor agonist for glycemic control and weight loss: From discovery to clinical proof of concept. Cell Metab 34:1234-1247 (2022) doi: 10.1016/j.cmet.2022.07.013.
- Jastreboff AM et al. Triple-hormone-receptor agonist retatrutide for obesity – A Phase 2 Trial.N Engl J Med Online ahead of print Jun 26. (2023). doi: 10.1056/NEJMoa2301972.
- Mansoor H et al. Effects of semaglutide on risk of cardiovascular events across a continuum of cardiovascular risk: combined post hoc analysis of the SUSTAIN and PIONEER trials. Cardiovasc Diabetol 19: 156 (2020) doi: 10.1186/s12933-020-01106-4
- Saha AK et al.Downregulation of AMPK accompanies leucine- and glucose-induced increases in protein synthesis and insulin resistance in rat skeletal muscle. Diabetes 59:2426-2434 (2010). doi: 10.2337/db09-1870.
- Sears B.The Zone. Regan Books. New York, NY. (1995)
- Sears B.Method of and nutritional and pharmaceutical compositions for reduction of hyperinsulinemia. U.S. Patent No. 6,140,304 (2000)
- Batterham RL et al. Critical role for peptide YY in protein-mediated satiation and body-weight regulation. Cell Metab 4:223-233 (2006). doi: 10.1016/j.cmet.2006.08.001.
- Ruderman NB et al. AMPK, insulin resistance, and the metabolic syndrome.J Clin Invest 123:2764-2772 (2013). doi: 10.1172/JCI67227
- Gonzalez A et al.AMPK and TOR: The Yin and Yang of cellular nutrient sensing and growth control. Cell Metab 31:472-492 (2020). doi: 10.1016/j.cmet.2020.01.015
- Christiansen CB et al. The impact of short-chain fatty acids on GLP-1 and PYY secretion from the isolated perfused rat colon.Am J Physiol Gastrointest Liver Physiol 315:G53-G65 (2018). doi: 10.1152/ajpgi.00346.2017
- Ludwig DS et al. High glycemic index foods, overeating, and obesity.Pediatrics 103:E26 (1999). doi: 10.1542/peds.103.3.e26.
- Larsen TM et al. Diets with high or low protein content and glycemic index for weight-loss maintenance.N Engl J Med 363:2102-13 (2010). doi: 10.1056/NEJMoa1007137.
- Johnston CS et al.Use of novel high-protein functional food products as part of a calorie-restricted diet to reduce insulin resistance and increase lean body mass in adults: A randomized controlled trial. Nutrients 9:1182 (2017). doi: 10.3390/nu9111182.
- Tettamanzi F et al.A high protein diet is more effective in improving insulin resistance and glycemic variability compared to a Mediterranean diet: A cross-over controlled inpatient dietary study. Nutrients 13:4380 (2021). doi: 10.3390/nu13124380.
- Vidal-Ostos F et al. Dietary protein and the glycemic index handle insulin resistance within a nutritional program for avoiding weight regain after energy-restricted induced weight loss Nutr Metab 19:71 (2022).doi: 10.1186/s12986-022-00707-y.
- Borja-Magno A et al. Differential effects of high dose omega-3 fatty acids on metabolism and inflammation in patients with obesity: eicosapentaenoic and docosahexaenoic acid supplementation. Front Nutr. 2023 May 5;10:1156995. doi: 10.3389/fnut.2023.1156995
- Alvarado J et al.A standardized maqui berry extract significantly lowers blood glucose and improves blood lipid profile in prediabetic individuals in a three-month clinical trial. Panminerva Med 58(Suppl 1):1-6 (2016). https://pubmed.ncbi.nlm.nih.gov/27820958/
- Davinelli S et al.A randomized clinical trial evaluating the efficacy of an anthocyanin-maqui berry extract on oxidative stress biomarkers. J Am Coll Nutr 34 (Suppl 1):28-33 (2015). doi: 10.1080/07315724.2015.1080108.
- Sears B and Saha AK.Dietary control of inflammation and resolution. Front Nutr 10:709435 (2021). doi: 10.3389/fnut.2021.709435.